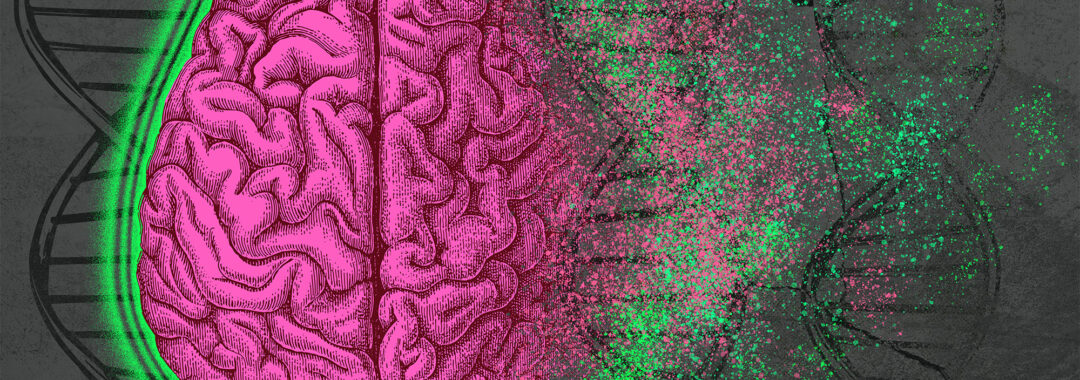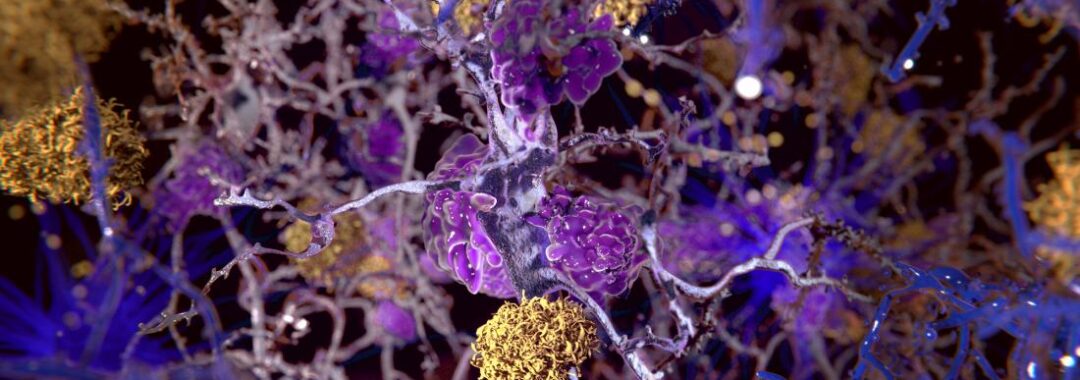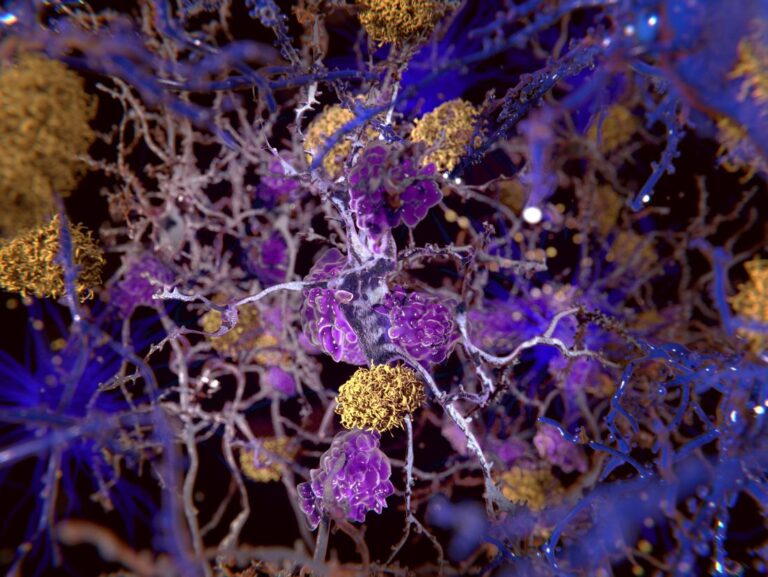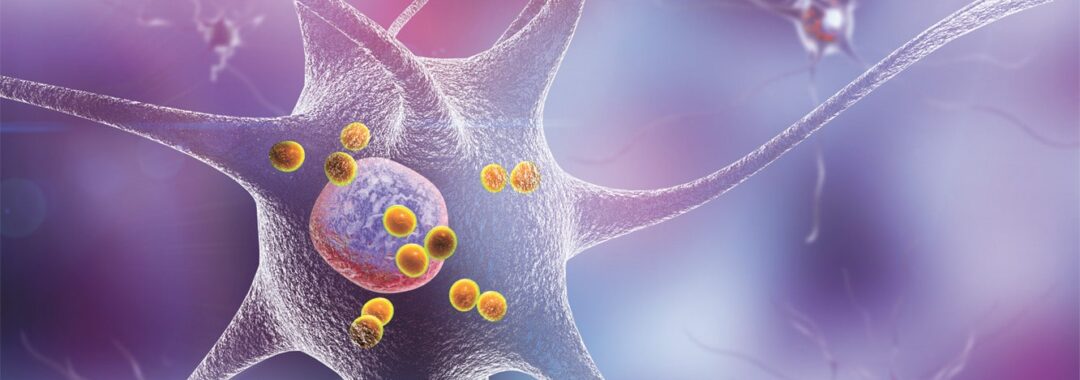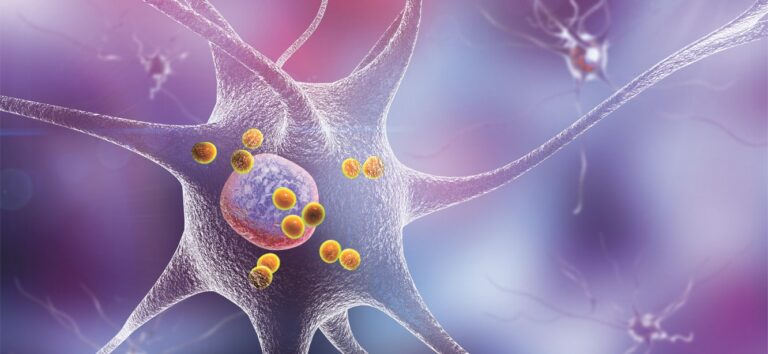
Differentiating between early Alzheimer’s disease (AD), and normal, age-related cognitive decline is difficult. To determine a diagnosis, biomarker assessments of amyloid plaques and neurofibrillary tangles (NFT) can be used.
AD is thought to be caused by elevated amyloid-beta protein (Aβ) that instigates NFT formation measured by pTau levels in the blood. As Aβ increases it forms Aβ plaques in the brain that precede memory problems by decades. Amyloid PET scans can assess Aβ levels while blood tests of pTau mirror Amyloid PET scans and have recently become accessible in clinical practice.
Preclinical AD is diagnosed when biomarkers are positive, but cognition is normal. Accumulation of Aβ first occurs in the frontal lobes causing multi-tasking difficulty in early AD. Memory issues follow when encoding circuit dysfunction occurs. As changes in the brain progress, neuronal death due to NFTs correlate to cognitive decline, but cognition should also be tested.
Cognitive tests assess memory, language, visuospatial skills, attention, and executive functioning. The pattern of these deficits in these areas differentiate AD from cognitive problems in normal aging. Mild cognitive impairment (MCI) or prodromal AD is diagnosed before the family says the patient is unsafe to live alone. That is when dementia is present, and the patient is said to have full blown AD.
Cognitive assessments are useful in assessing patients at all stages of decline. These tests are widely available. Immediate recall and delayed recall are assessed by examining the ratio between immediate and delayed recall to diagnose early AD compared to using total recall or only delayed recall. Cognitive measures also examine semantic memory. This is the memory of acquired knowledge such as words and facts, which can be one of the first areas affected before MCI is diagnosed. Verbal fluency tasks such as naming items within a category or beginning with a specific letter can be predictive of MCI.
Episodic memory is encoded through the Papez circuit. When there is a failure in this circuit, there is difficulty learning new information because a person is unable to encode the information, meaning that providing the information multiple times will not improve their performance. Learning is always intact in normal aging; normal ‘forgetfulness’ is due to a retrieval deficit where a person is unable to retrieve information they have previously learned. Neuropsychology tests can identify a retrieval deficit versus an encoding deficit.
Determining a diagnosis of AD is a result of a variety of tools. Biomarkers examined through imaging and blood tests can aid in diagnosis before MCI is first noticed. Cognitive testing gives insight into memory and other cognitive dysfunction and is helpful in monitoring the progression of MCI and AD. Early diagnosis is advantageous as we continue to research treatments. Biomarker tests are becoming more widely available for people to understand their risks of developing AD during the preclinical stage. There is still much more progress to be made, but these tools offer an initial step in preventing decline in AD.
Sources
Bruno, D., Jauregi Zinkunegi, A., Pomara, N., Zetterberg, H., Blennow, K., Koscik, R. L., … & Mueller, K. D. (2023). Cross-sectional associations of CSF tau levels with Rey’s AVLT: A recency ratio study. Neuropsychology, 37(6), 628.
Caselli, R. J., Locke, D. E., Dueck, A. C., Knopman, D. S., Woodruff, B. K., Hoffman-Snyder, C., … & Reiman, E. M. (2014). The neuropsychology of normal aging and preclinical Alzheimer’s disease. Alzheimer’s & Dementia, 10(1), 84-92.
De Jager, C.A., Hogervorst, E., Combrinck, M., & Budge, M.M. (2003). Sensitivity and specificity of neuropsychological tests for mild cognitive impairment, vascular cognitive impairment and Alzheimer’s disease. Psychological Medicine, 33(6), 1039-1050.
DeTure, M.A., & Dickson, D.W. (2019) The neuropathological diagnosis of Alzheimer’s disease. Molecular Neurodegeneration, 14(32). https://doi.org/10.1186/s13024-019-0333-5
Hill, Carrie (2022, November 11). Neuropsychological Testing to Evaluate Alzheimer’s Disease. Verywell Health. https://www.verywellhealth.com/neuropsychological-testing-alzheimers-disease-98062.
National Institute on Aging. (2023, November 22). Memory Problems, Forgetfulness, and Aging. National Institue of Health. https://www.nia.nih.gov/health/memory-loss-and-forgetfulness/memory-problems-forgetfulness-and-aging.
Rasmussen, J., & Langerman, H. (2019). Alzheimer’s disease–why we need early diagnosis. Degenerative neurological and neuromuscular disease, 123-130.
Wright, L. M., De Marco, M., & Venneri, A. (2022). Verbal fluency discrepancies as a marker of the prehippocampal stages of Alzheimer’s disease. Neuropsychology, 37(7), 790-800.