We recently introduced the gut-brain axis as a bidirectional communication loop. Our bodies control, yet are in part controlled, by the living microorganisms within our gut. An irregularity at either end of the gut-brain axis often leads to poorer health, so are there ways to ensure a healthy microbiome? Welcome to part 3!—The final chapter of our series where we discuss what we can do to ensure gut health!
Diet is a key mediator of your microbiome. Foods high in fiber, changes in fat intake, and timing of meals all effect the microbiome components and its function. Humans consuming a Mediterranean diet (MD) boosted their microbiome diversity compared to their western diet (WD) counterparts. The MD consists of large amounts of plant-based foods and a higher proportion of monosaturated fats, rather than the WD which contains high amounts of saturated fats, animal proteins, and sugars. Diets high in grains, vegetables, beans, nuts, and the like appear to be healthiest for our gut microbiome.
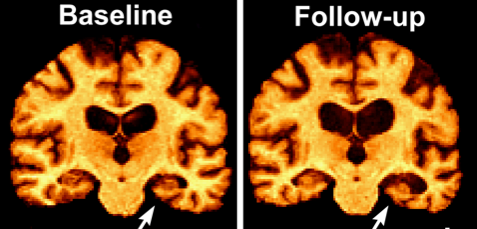
Fecal samples were analyzed from individuals with (Alzheimer’s disease) AD and those without to categorize metabolites associated with AD. Metabolites, or postbiotics, are byproducts given off by our gut microbes as they digest our food. A ranking of grouped foods was created based on their strength of association to AD. Interestingly, the healthiest food rankings not associated with AD approximately mirror the MD food pyramid, emphasizing the importance of a proper diet for microbiome and overall host health.
The internal process regulating our sleep-awake cycle is called the circadian rhythm, making it natural for us to experience half of our 24-hour day active and feeding versus the other half resting and fasting. With the development of artificial lights, humans are no longer bound to feeding only during the light phase of the day. Emerging preclinical research suggests that our gut microbiome maintains a similar circadian rhythm to us, evoking the importance of eating patterns like frequency and timing of food intake. Night shift workers that consume their meals at night are at a 40%-60% increased risk of developing obesity and metabolic syndrome, indicating how important it is for our health to adhere to our circadian rhythm, which is largely dictated by the sun. Furthermore, adding light to the night cycle of mice results in metabolism disruption, with an increased body mass index (BMI) and insulin resistance compared to mice with a proper dark/light cycle, suggesting the importance of a consistent night of sleep with minimal disruption.
Probiotics are living microorganisms that provide health benefits when consumed in adequate quantity. Although found naturally, like in yogurts and sauerkraut, they’re most often consumed as an over the counter (OTC) supplement not requiring FDA regulation. Prebiotics are additional OTC supplements taken with probiotics and contain plants and grains to support the probiotic strains growth and establishment in the gut. These supplements are filled with a variety of bacterial strains thought to be beneficial, like Lactobacillus, and Bifidobacterium. In humans, broad-spectrum probiotics attenuated stress-induced reductions in cognition, but had no effects in the absence of stress. Probiotics were also shown to reduce depressive symptoms in individuals with irritable bowel syndrome (IBS). Diabetic individuals taking probiotics improve their brain functioning and synaptic activity compared to diabetics not taking probiotics.
Chronic ingestion of fermented milk with probiotics was associated with reduced task responsiveness in humans compared to those on control treatment. Other studies show no difference in microbiome compilation or cognition in individuals using pre- and probiotics compared to those not. Unfortunately, our current understanding of pre-and probiotics ranges is scarce indicating the need for further research identifying harmful and beneficial strains in
those that are healthy and diseased.
Fermented foods and drinks like kimchi and kombucha are rich in probiotics. Kombucha, made by fermenting tea and sugar with live bacteria and yeast, originated in China around 220 B.C.. It’s worldwide popularity has recently increased with the understanding of how integral our microbiomes are for our health. Since 2017, kombucha and other probiotic drink sales increased by almost 40% and is currently considered the fastest growing product in the functional beverage market.
So does it work?
In animal studies the probiotic drink shows evidence of anti-tumor and anti-cancer properties, and can help to inhibit neurodegenerative diseases. Unfortunately, no controlled studies with human subjects have shown any evidence of these benefits indicating the need for regulated clinical trials. Yet, the consumer market would have you believe otherwise. Luckily, it’s not considered harmful if consumed by a healthy individual at 4oz. or less per day. However, it does contain small amounts of alcohol and is therefore not recommended for pregnant women.
Smoking and drinking have historically been known to harm the lungs and heart, but it turns out the damage is more systemic than that. Smoking induced alterations of the microbiome resemble those of obesity and inflammatory bowel disease (IBD). The cessation of smoking reversed the microbiome changes indicating that kicking the habit could return your gut to better health. Alcohol reduces bacteria with anti inflammatory activity within the gut. Alcohol and smoking both negatively affect the microbiome.
AD drugs that inhibit the acetylcholinesterase enzyme have negative effects on rat microbiomes demonstrating that some AD drug treatments may lead to a worsening of AD pathology long-term. Although current AD drugs temporarily relieve the symptoms associated with the disease they tend to lose efficacy rather quickly, generally in a span of a couple years. The use of pre- and probiotics in conjunction with AD treatments may prevent or correct this gut dysbiosis allowing the therapeutic effects to be exploited more completely. Drugs like antibiotics decrease microbial diversity and can allow for the overpopulation of bad microbes within the gut which may also be prevented by pre- and probiotics.
Our lifestyle has great capacity in determining our gut microbial health, which in turn affects our comprehensive health. We have the ability to maintain or modify our regiments, staying or becoming healthier by choosing good habits, like eating a proper diet. Considering the gut microbiome has vast local and systemic effects, it’s possible the future will be filled with a large variety of probiotics used to treat most any ailment, but for now more research is needed. Identifying what the good and bad microbes are still needs clarification, in addition to what makes them such. Clinical trials with the determined good microbes as treatment may then be better established. Until then, keep your diet lean and regular, don’t smoke or drink, and get good sleep routinely! Until next time!