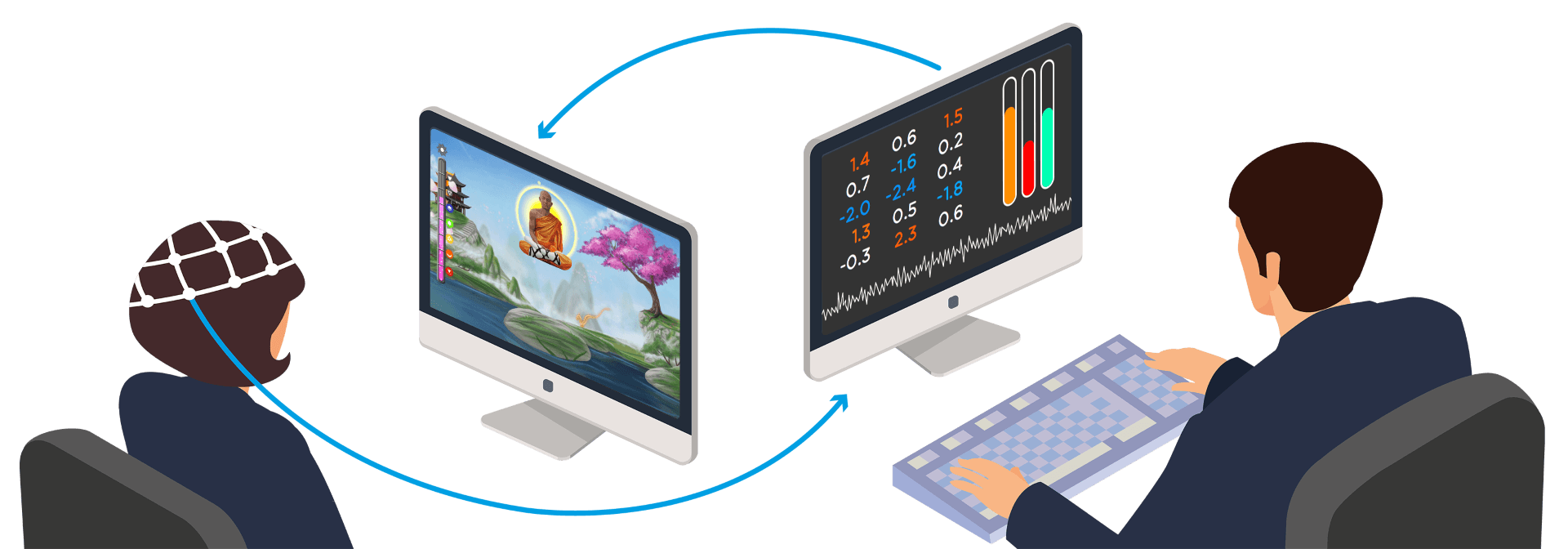
Our response to stimuli may be detrimental to our health and cognition, like being stressed while driving in traffic. Neurofeedback retrains our physiologic response to stressful situations, by measuring our brain waves and modifying them in a desirable manner. These waves have been classified into 4 types:
Delta: Delta waves are what we experience when we are sleeping.
Theta: Associated with a “daydream” like state in which cognitive efficiency is reduced.
Alpha: Correlates to a state of relaxation, essentially the brain is “idling” and not currently engaged but ready to respond if needed.
Beta: Associated with active mental/intellectual activity and outward concentration on the task(s) at hand.
During normal aging, brain activity shifts with increasing delta and theta waves in patients with Alzheimer’s disease (AD) a larger increase in theta activity with reduced alpha/beta activity is seen. Neurofeedback trains patients to consciously control their neural activity, increasing alpha/beta activity and decreasing delta/theta activity. Those practiced in neurofeedback can “activate” their own brain to be more engaged and capable of focusing on tasks requiring complex cognition, and possibly alleviating AD symptoms.
Neurofeedback training was assessed in individuals with probable AD also taking cholinesterase inhibitors. Half were also treated with neurofeedback training while the other half just received treatment as usual (TAU), with cognitive testing occurring pre- and post- treatment. Neurofeedback training sessions began within two weeks of pre-treatment testing. Sessions occurred twice a week for 15 weeks, during which participants watched a movie while receiving an electroencephalography (EEG). If the training worked (e.g. increased neural activity) the movie was shown in a higher contrast (visual cue) and the participant heard a beep (auditory cue) to notify/reward them. After completion of all training sessions, participants were re-tested and administered cognitive assessments.Patients receiving neurofeedback training had higher total cognitive testing scores, including improved orientation and memory compared to the untreated group. The neurofeedback group showed an improvement in memory and learning with no improvement or decline in other areas compared to their pretreatment scores. The TAU group declined in total cognitive scores in all areas except orientation in time.
These results suggest that neurofeedback training is effective in preventing cognitive decline for AD patients. While these results are promising, previous studies show conflicting results. In one study, both neurofeedback training and placebo improved attention, executive function and memory suggesting that this may have been a ”placebo effect”. In another study that trained to increase alpha power, participants experienced an improvement in memory and cognitive performance. Admittedly, each study had slightly different treatment goals, which may have contributed to these differential results. In order to concretely confirm the efficacy of neurofeedback training in AD, further research is required.
